Case study: muscle twitching
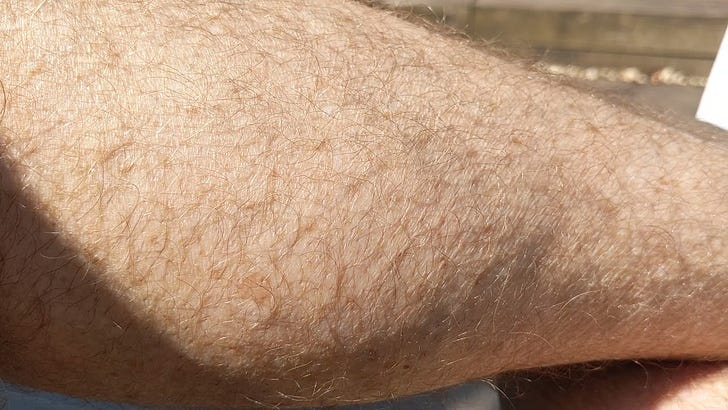
A 58-year-old marathon runner complains of visible muscle twitching in both his calves after running. Does he have motor neuron disease (MND)?
Case
A 58-year-old marathon runner complains of visible muscle twitching in both his calves after running. When asked he says he can’t feel the twitching it is only noticeable when looking at his calves.
What is the diagnosis?
Spontaneous Muscle Activity
There are several syndromes for involuntary muscle twitching or muscle activity. In general, you need to decide if the twitching is localised/focal or generalised/diffuse. Focal muscle twitching is likely to be myokymia or fasciculation.
Myokymia
Myokymia is continuous involuntary rippling or worm-like movements of the muscle.
Myokymia is a spontaneous electrical activity characterized by grouped discharges of motor unit action potentials. Because it activates several motor units patients can feel the twitching or muscle rippling. Localised or focal myokymia is very common in the general population and is usually benign and can be triggered by overexertion, caffeine consumption or lack of sleep.
In healthy individuals, eyelid myokymia is common, causing twitches in the orbicularis oculi muscles.
Pathological myokymia typically originates from areas of axonal demyelination and in this situation the myokymia is more diffuse, for example, facial myokymia from a brainstem demyelination lesion in patients with multiple sclerosis and can also be seen in some focal demyelinating neuropathies. Limb myokymia is observed with radiation plexopathies and is a delayed complication of radiation therapy and is often found on EMG only.
Generalised myokymia can be seen in acute inflammatory neuropathies such as Guillain–Barre, chronic inflammatory neuropathies, for example, chronic inflammatory demyelinating polyneuropathy (CIDP), uremia, thyrotoxicosis, neuromyotonia or Isaac's syndrome, exercise-induced myokymia, timber rattlesnake venom, gold therapy or hereditary episodic ataxia.
Myokymia produces irregular discharges of slow frequencies, averaging 0.1 to 3 Hz. The audio signal of myokymia is ‘marching.’
Treatment of benign myokymia is usually unnecessary as it is asymptomatic or self-limited. For pathological myokymia, treatment is for the underlying condition.
Fasciculations
Fasciculations are spontaneous, involuntary contractions of a single motor unit, a part of it, or of several motor units. When the unit is large enough, or close enough to the surface, the fasciculations may be visible but are too small to be felt. The exception to the latter is macro-fasciculations which occurs when very large motor units fire. The latter is seen in conditions such as the post-polio syndrome when surviving motor units are expanded due to axonal sprouting to innervate a very large number of motor fibres.
The discharges associated with fasciculations occur irregularly and might be found in EMGs of healthy individuals (benign fasciculations of the calf). Nevertheless, the occurrence of fasciculations, similarly to fibrillations, can be due to denervation and present as a sign of motor neuron diseases and pathologies affecting the motor nerve more proximally, i.e. close to the anterior horn cell, for example, motor radiculopathies or some forms of multifocal demyelinating motor neuropathies.

Normal EMG
The EMG is a useful tool in assessing the electric activity of motor units using a small electrode.
A motor unit includes:
An anterior horn cell.
The cell’s axon and terminal branches.
Neuromuscular junctions.
The muscle fibres innervated by the terminal branches.
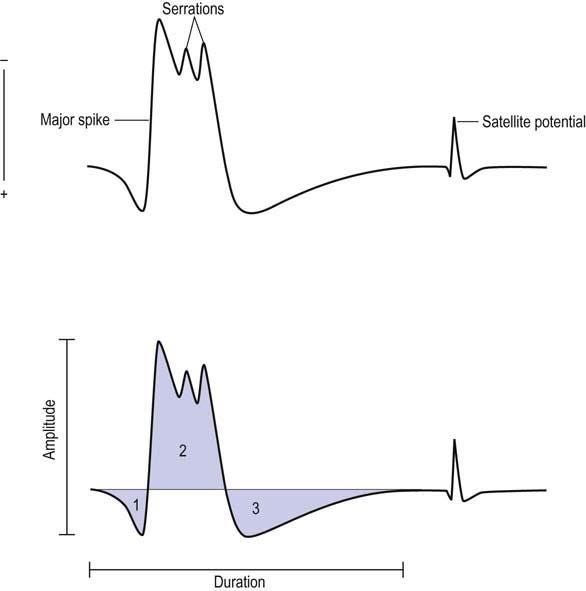
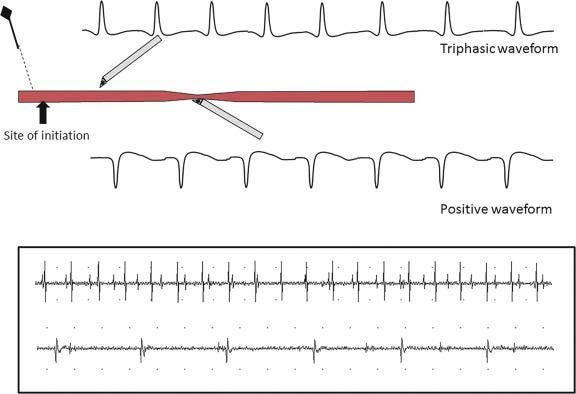
An EMG records the triphasic action potential of the motor unit, consisting of a positive (downward) phase, a negative (upward) phase, and an additional positive phase, reflecting the movement of the electrical impulse as recorded, or “seen”, by the EMG needle.
At rest, healthy muscle fibres are electrically silent. Upon movement, motor units are recruited, depicted as waves of different frequencies.

Fibrillations
Fibrillations represent the action potentials of a single muscle fibre due to denervation. This could be the result of any nerve damage, as part of neurologic, inflammatory, or dystrophic muscle diseases. Fibrillations cannot be observed visually, and are merely an electrical sign. They may occur for a long period following the nerve damage and are characterized by a regular firing pattern, with firing frequencies of < 1 Hz to about 15 Hz.
Our Case
As our patient describes visible muscle twitching without feeling the twitching it is likely he has exercise-induced benign fasciculations of the calf. Further questioning and a detailed neurological examination are required to exclude generalised fasciculations, with associated muscle wasting and weakness. The latter is to exclude the possibility of a more sinister underlying pathology, in particular motor neurone disease.
Sources
UpToDate – Overview of Electromyography
Mills KR. The basics of electromyography. Journal of Neurology, Neurosurgery & Psychiatry. 2005 Jun 1;76(suppl 2):ii32-5.
Rubin DI. Normal and abnormal spontaneous activity. Handbook of clinical neurology. 2019 Jan 1;160:257-79.
Author
Sapir Dreyer
Year 6 medical student
Hebrew University, Jerusalem
sapirdreyer@gmail.com