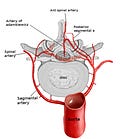
Paraparesis post-surgery
On coming around from the anaesthetic he cannot move his legs and has a sensory level at approximately T4. What is the diagnosis?
A 54-year-old man presents in A&E with severe abdominal pain. He is found to have a leaking abdominal aortic aneurysm (AAA) and undergoes emergency surgery. On coming around from the anaesthetic post-surgery, he cannot move his legs and has a sensory level at approximately T4.
Questions
What other information do you need clinically to make a bedside diagnosis?
What is the most likely diagnosis?
What anatomical factor explains a sensory level at T4?
What is his prognosis?
Answers
What other information do you need clinically to make a bedside diagnosis?
The state of his posterior column function. Is his joint position and vibration sense intact? If yes, the syndromic diagnosis is an anterior spinal cord syndrome: loss of motor function (corticospinal tract) and spinothalamic sensation (pin-prick, tickle, light touch and temperature) with preservation of posterior column function.
What is the most likely diagnosis?
Anterior spinal artery syndrome from hypoperfusion or occlusion of the artery of Adamkiewicz. The artery of Adamkiewicz is the largest anterior segmental artery supplying the lower two-thirds of the spinal cord and typically arises from a left posterior intercostal artery at the level of the 9th to 12th intercostal arteries, which are branches from the aorta.
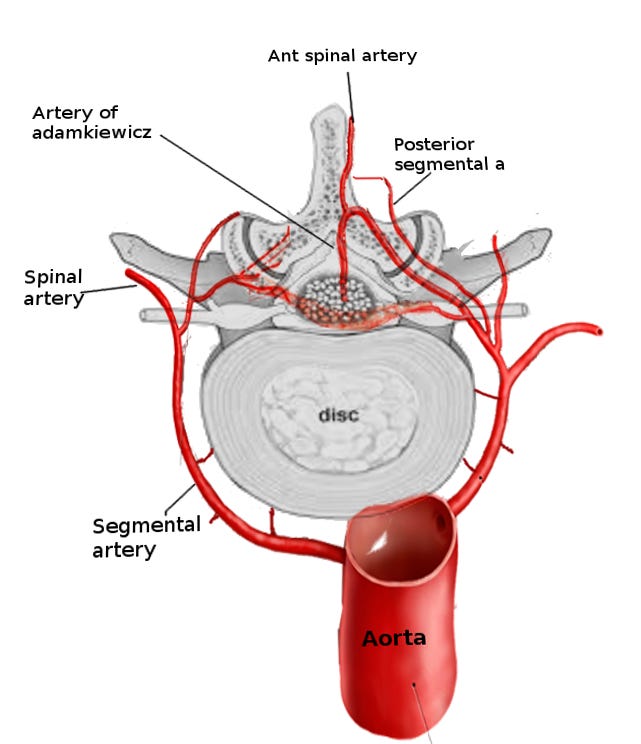
What anatomical factor explains a sensory level at T4?
This is within the so-called watershed area of the main arterial supply to the anterior spinal cord. The artery of Adamkiewicz supplies the lower two-thirds of the spinal cord via the anterior spinal artery. The upper third of the cord is also supplied by the anterior spinal artery, which is formed from branches from the two vertebral arteries. The longitudinal or craniocaudal spinal cord watershed, i.e. between these two arterial territories, is typically between T4 and T6, but this can vary depending on the individual’s anatomy and whether or not there is a well-developed collateral blood supply.
What is his prognosis?
The long-term prognosis of anterior spinal cord syndrome is generally poor, but a small proportion of patients can make a relatively good recovery, i.e. become fully independent and mobile. Spinal cord infarction has an overall mortality rate of 9 to 23% and usually occurs shortly after the injury (Sandoval and De Jesus, 2021). A review of patients with spinal cord infarction reported that 24% did not improve, and only 20% improved significantly (Cheshire et al., 1996). However, other series report that only 1-5% recovered completely (Foo & Rossier, 1983; Kumral et al., 2011).
Extra-reading
Sandoval and De Jesus. Anterior Spinal Artery Syndrome. Stat Pearls. Last Update: August 30, 2021.
Recommended work and further revision
Create a virtual case study covering (i) complete, (ii) hemi-cord (Brown-Sequard syndrome) and (iii) central spinal cord syndromes.
How do you differentiate (i) a conus syndrome and (ii) a cauda equina syndrome from a spinal cord syndrome?
Review the functional anatomy and blood supply of the spinal cord.
Review the following fibre tracts:
Corticospinal tract
Spinothalamic tract
Posterior columns
Review the cutaneous dermatomes.
Why is a sensory level on the upper chest so important?
How do neuro, spinal or vascular surgeons assess the functional state of the spinal cord in a patient undergoing surgery?
Please answer these questions in the comments section.
References
General Disclaimer: Please note that the opinions expressed here are those of Professor Giovannoni and do not necessarily reflect the positions of Barts and The London School of Medicine and Dentistry nor Barts Health NHS Trust.