Case study
A 69y old former office worker presented to the emergency department with acute onset frontal headache that reached its peak in 30 seconds. The left eye was completely shut but not proptosed and the pupil was unresponsive to all modalities. There was nausea, moderate neck stiffness and pyrexia. Acuity in the left eye was reduced to counting fingers and the right upper temporal field was reduced to confrontation.
Past history: chronic obstructive pulmonary disease. Myocardial infarction 10 years previously. Hypertension that was well controlled and raised cholesterol
What is the most likely diagnosis?:
Giant anterior communicating artery aneurysm
Pituitary apoplexy
Giant cell arteritis
Acute sphenoid sinus infection
Cavernous sinus thrombosis
Learning points
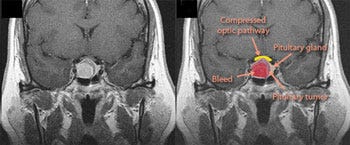
Diagnosis: Pituitary apoplexy presenting with thunderclap headache.
Giant anterior communicating artery aneurysms rarely cause blindness but they may compress the pituitary gland if they are smaller and downward pointing. Giant cell arteritis (GCA) may cause thunderclap headache but this is rare. More likely there is a chronic dull pain with nodules along the course of the superficial temporal arteries associated with tongue or jaw claudication and symptoms of polymyalgia rheumatica. Visual loss can be acute but complete ophthalmoplegia is rare. Acute sphenoid sinus infection seldom causes thunderclap headache and may affect the pituitary gland but not the optic nerve. Optic nerve involvement is characteristic of infection of the ethmoid sinus, given the proximity of the optic nerves to this sinus. Cavernous sinus thrombosis presents with acute ophthalmoplegia and proptosis but not severe visual impairment. Any visual loss is due to venous congestion in the retina. Thunderclap headache is well recognised in thrombosis of the other cerebral venous sinuses but it has not been described so far in cavernous sinus thrombosis.
The presentation here is that of thunderclap headache which is defined as pain reaching its maximum intensity within 60 seconds. There is a broad differential diagnosis for thunderclap headache but here the major localising clues are the unilateral blindness and ophthalmoplegia. In pituitary apoplexy there is acute haemorrhage into an enlarged pituitary gland causing pressure on surrounding structures namely: the optic chiasm which lies above the pituitary gland; cranial nerves III, IV, V and VI which lie within the cavernous sinus. Neck stiffness relates to leakage of blood into the subarachnoid space.
Red flag: neck stiffness in pituitary apoplexy may result in a mistaken diagnosis of meningitis. A lumbar puncture could be hazardous.
Asymmetrical chiasmal pressure explains the blindness in the left eye and contralateral upper temporal field (see Chapter 2). It is likely the patient had a post-fixed chiasm such that pressure from the pituitary gland compressed a) the left optic nerve resulting in ipsilateral blindness and b) the lower nasal retinal fibres in the chiasm that sweep forward into the optic nerve causing an upper temporal field loss in the (contralateral) right eye - the junctional scotoma.
Red flag: a blind eye with ophthalmoplegia is unlikely to be cavernous sinus thrombosis. This happens because the optic nerves and chiasm are outside the cavernous sinus.
Handle: Thunderclap headache with unilateral blindness and ophthalmoplegia is pituitary apoplexy
The patient was treated with steroids and antibiotics. The pituitary gland was removed by trans-sphenoidal approach and the patient recovered well. He was discharged on cortisone and thyroxine.
By Professor Chris Hawkes